We offer a family room to you and your partner/companion where the staff will be available to guide and help you according to your needs.
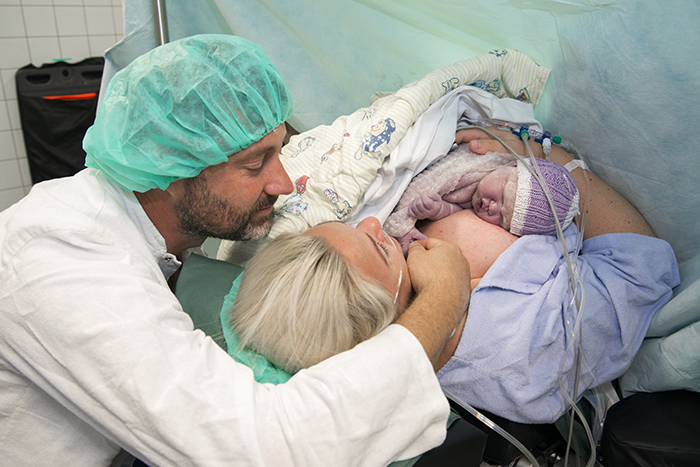
We recommend that your partner or companion stay with you in order to create the best conditions for getting to know your new baby together.
The expected admission time is 1-2 nights.
Get out of bed as quickly as possible
Within 6 hours after the caesarean section you will need to get out of bed for the first time in order to "restart" your body after the operation. Please take a walk in the ward as quickly as possible.
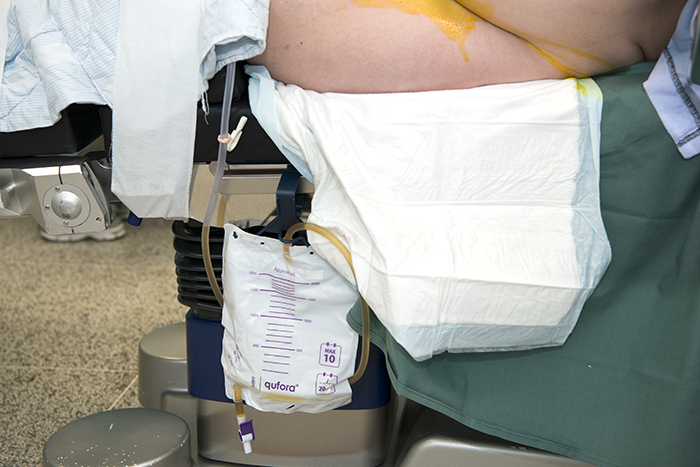
The catheter in your bladder will be removed at the latest 6 hours after the operation.
During the days following the caesarean section it is important that you mobilize and rest alternately. It is advisable that you get out of bed for a couple of hours in the morning, in the afternoon, and in the evening.
You can take a shower whenever you feel like it.
The bandage will stay on for 6-7 days after the caesarean section. If it detatches in the shower, you won't need to put on a new one.
Normally, you will be able to take care of your baby yourself.
Food and drink
You may eat and drink whatever you prefer. If you have allergies or don't eat special types of food, please let the nurses know.
Treatment of pain
After the caesarean section you will experience pain in the wound and contractions in your uterus (after-pains).
We recommend that you receive pain-relieving tablets routinely and regularly ensuring that you will not experience sudden pain when the tablets stop working.
The treatment consists of Paracetamol, Ibuprofen and additionally Morphine if needed.
Urination after spinal anaesthesia
It is important that you experience normal urination 3-4 hours after the catheter has been removed from your bladder.
You may not experience the urge to urinate during the first couple of days after the spinal anaesthesia and therefore you should pay extra attention to emptying your bladder.
We recommend that you try to urinate every 3-4 hours. Please contact the staff if problems with urination occures.
If the bladder becomes too distended, the uterus may have trouble contracting properly and thereby raising the risk of increased bleeding. A distended bladder may also cause long term complications.
Bowel function
Mobilization is important to get your bowels started again. This is one of the reasons why we recommend you get up and walk around.
Drink plenty of water and eat lots of fibers and vegetables – this promotes the process.
You will receive a mild laxative the first couple of days after the caesarean section. If you have experienced constipation during your pregnancy it may be a good idea to take Magnesia tablets a couple of days before the caesarean section. Magnesia is a "over-the-counter" medicine.
Guidance on rehabilitation
Postnatal exercise is just as important after a caesarean section as after a vaginal delivery.
The muscles of the pelvic floor need to be rehabilitated and re-trained as they have been affected by the pregnancy. The entire body needs help to change from pregnancy to normal mode again.
We recommend that you lift only to your pain threshold the first 6 weeks after the caesarean section. As a guideline this corresponds to the weight of the baby and the carrycot or baby car seat.
Breastfeeding guidance
You are encouraged to contact the staff at breastfeedings to receive guidance on correct suckling technique, breastfeeding positions etc.
We add on to the knowledge you already have from your antenatal classes or the experience you have from breastfeeding previously.
Doctor's examination
You do not normally need an examination after a caesarean section but it is possible to contact a doctor if needed.
The majority will however see a doctor or a medical student during their stay and have the opportunity to discuss the operation. Feel free to request a medical consultation.
 Your preparations for the surgery
Your preparations for the surgery


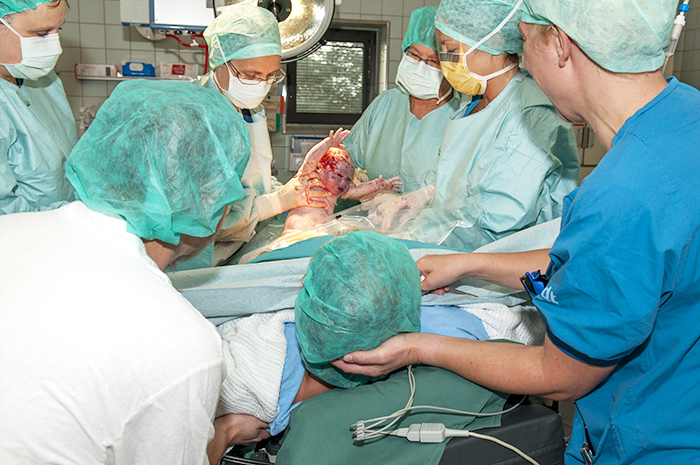
 About the surgery
About the surgery

 Risks and side effects
Risks and side effects
 After surgery but still in hospital
After surgery but still in hospital
 When you come home
When you come home
 Further healthcare appointments
Further healthcare appointments
 Contact
Contact